- Study results from investigational
agents Opdivo (nivolumab), elotuzumab, and ulocuplumab, as well as
Sprycel (dasatinib), will be highlighted
- First presentation of data for
Opdivo in Hodgkin lymphoma and non-Hodgkin lymphoma, and final
Phase 2 results of elotuzumab in multiple myeloma highlight
potential of immuno-oncology in hematologic malignancies
- Breadth of program demonstrates
company’s growing commitment to the field of hematology through
immuno-oncology leadership
Bristol-Myers Squibb Company (NYSE:BMY) today announced that
study results on investigational agents Opdivo (nivolumab), a PD-1
immune checkpoint inhibitor, elotuzumab, an antibody targeted
against Signaling Lymphocyte Activation Molecule (SLAMF7),
ulocuplumab, an anti-CXCR4 antibody, and Sprycel (dasatinib), will
be featured in oral presentations at the 56th annual meeting of the
American Society for Hematology (ASH) in San Francisco from
December 6-9, 2014. Data will be presented in multiple hematologic
malignancies, including Hodgkin lymphoma (HL), non-Hodgkin
lymphoma, multiple myeloma, chronic-phase chronic myeloid leukemia
(CP-CML), acute myeloid leukemia (AML) and T-Cell acute
lymphoblastic leukemia. In May 2014, the U.S. Food and Drug
Administration (FDA) granted Opdivo its first Breakthrough Therapy
Designation for the treatment of patients with HL after failure of
autologous stem cell transplant and brentuximab.
“The breadth of data we are presenting at ASH this year,
including data on ulocupumab and findings from our immuno-oncology
development programs for Opdivo and elotuzumab, underscores our
commitment to research and development in hematology and to
improving outcomes for patients across a range of blood cancers,”
said Michael Giordano, senior vice president, Head of Development,
Oncology, Bristol-Myers Squibb.
Opdivo (nivolumab) Oral
Presentations in HL and Lymphoid Malignancies
Data on Opdivo, an investigational PD-1 immune checkpoint
inhibitor, will be presented during two oral presentations on
Monday, December 8. At 7:00 a.m. PST, preliminary efficacy, safety
and biomarker results will be presented from the relapsed or
refractory HL cohort of CheckMate - 039, a Phase 1 dose escalation
study of patients with relapsed or refractory hematologic
malignancies (Abstract #289). At 7:30 a.m. PST, additional results
from CheckMate-039 will be presented, including patients with
relapsed or refractory non-Hodgkin lymphoma (Abstract#291).
Elotuzumab Oral Presentation in
Multiple Myeloma
Final results from the Phase 1b/2 study of elotuzumab in
combination with lenalidomide and dexamethasone in patients with
relapsed or refractory multiple myeloma will be presented in an
oral session on Monday, December 8 at 7:15 a.m. PST (Abstract
#302).
In May 2014, the FDA granted elotuzumab Breakthrough Therapy
Designation for use in combination with one of the commonly used
chemotherapy treatments for multiple myeloma (lenalidomide, used in
combination with dexamethasone) in patients who have received one
or more prior treatments.
Sprycel (dasatinib) Oral
Presentations in CP-CML
Results from two Sprycel studies will be highlighted in oral
presentations, including five-year data from the Phase 3 trial,
DASISION, comparing Sprycel to Gleevec® *(imatinib mesylate) in
newly diagnosed CP-CML patients on Sunday, December 7 at 4:45 p.m.
PST (Abstract #152) and seven-year data from a Phase 3 study of
patients with Gleevec-resistant or intolerant CP-CML on Monday,
December 8 at 3:30 p.m. PST (Abstract #520).
* Gleevec is a registered trademark of Novartis AG
Additional Data
Presentations
Results from a Phase 1 study in relapsed/refractory AML,
including safety, tolerability and clinical activity of the
investigational anti-CXCR4 antibody ulocuplumab will be presented
for the first time during an oral presentation on Monday, December
8 at 10:45 a.m. PST (Abstract #386). Additionally, results from a
Phase 1 study of the safety and activity of BMS-906024, a notch
inhibitor, in patients with relapsed T-Cell acute lymphoblastic
leukemia, will be presented during a poster session on Saturday,
December 6 between 5:30 and 7:30 p.m. PST (Abstract # 968).
Full session details of the 2014 Annual Meeting can be accessed
on the ASH website:
http://www.bloodjournal.org/ash-annual-meeting-abstracts?sso-checked=true
About Opdivo
Cancer cells may exploit “regulatory” pathways, such as
checkpoint pathways, to hide from the immune system and shield the
tumor from immune attack. Opdivo is an investigational, fully-human
PD-1 immune checkpoint inhibitor that binds to the checkpoint
receptor PD-1 (programmed death-1) expressed on activated
T-cells.
Bristol-Myers Squibb has a broad, global development program to
study Opdivo in multiple tumor types consisting of more than 35
trials – as monotherapy or in combination with other therapies – in
which more than 7,000 patients have been enrolled worldwide. Among
these are several potentially registrational trials in non-small
cell lung cancer (NSCLC), melanoma, renal cell carcinoma (RCC),
head and neck cancer, glioblastoma and non-Hodgkin lymphoma.
In 2013, the FDA granted Fast Track designation for Opdivo in
NSCLC, melanoma and RCC. In April 2014, the company initiated a
rolling submission with the FDA for Opdivo in third-line
pre-treated squamous cell NSCLC and expects to complete the
submission by year-end. The FDA granted Opdivo its first
Breakthrough Therapy Designation in May 2014 for the treatment of
patients with Hodgkin lymphoma after failure of autologous stem
cell transplant and brentuximab. On July 4, Ono Pharmaceutical Co.
announced that Opdivo received manufacturing and marketing approval
in Japan for the treatment of patients with unresectable melanoma,
making Opdivo the first PD-1 immune checkpoint inhibitor to receive
regulatory approval anywhere in the world. On September 26,
Bristol-Myers Squibb announced that the FDA accepted for priority
review the Biologics License Application (BLA) for previously
treated advanced melanoma, and the Prescription Drug User Fee Act
(PDUFA) goal date for a decision is March 30, 2015. The FDA also
granted Opdivo Breakthrough Therapy status for this indication. In
the European Union, the European Medicines Agency (EMA) has
validated for review the Marketing Authorization Application (MAA)
for Opdivo in advanced melanoma. The application was also granted
accelerated assessment by the EMA’s Committee for Medicinal
Products for Human Use (CHMP). The EMA also validated for review
the MAA for nivolumab in NSCLC.
Bristol-Myers Squibb has proposed the
name Opdivo (pronounced op-dee-voh), which, if approved
by health authorities, will serve as the trademark for
nivolumab.
About Elotuzumab
Elotuzumab is an investigational antibody targeted against
Signaling Lymphocyte Activation Molecule (SLAMF7), a protein found
on the surface of myeloma cells and Natural Killer (NK) cells,
plasma cells and other immune cells, but not detectable in normal
tissue. Based on current research, elotuzumab appears to have
different effects when it binds to SLAMF7 on different cell types.
The company is investigating whether through both direct activation
and engagement of NK cells, elotuzumab may selectively target and
kill SLAMF7 expressing myeloma cells.
Elotuzumab is being studied in combination with lenalidomide and
low-dose dexamethasone in untreated multiple myeloma (ELOQUENT 1
study) as well as in multiple myeloma that has relapsed or no
longer responds to treatment (ELOQUENT 2 study). It is also being
studied as a single agent in smoldering multiple myeloma, which is
a slow growing, early form of myeloma, as well as additional
studies looking at elotuzumab in combination with different
chemotherapies that are commonly used to treat myeloma at different
stages of the disease.
In May 2014, the U.S. FDA granted elotuzumab Breakthrough
Therapy Designation for use in combination with one of the commonly
used chemotherapy treatments for multiple myeloma (lenalidomide,
used in combination with dexamethasone) in patients who have
received one or more prior treatments. Elotuzumab is being
co-developed with AbbVie, with Bristol-Myers Squibb leading the
commercialization of the agent.
About Sprycel
Sprycel was first approved by the FDA under accelerated review
for the treatment of adults with CP Ph+ CML who are resistant or
intolerant to prior therapy including imatinib in 2006. At that
time, Sprycel was also approved for adults with Ph+ acute
lymphoblastic leukemia (ALL) who are resistant or intolerant to
prior therapy. Full approval was granted in May 2009. It is the
first and only kinase inhibitor with survival data in its label for
CP Ph+ CML patients who are resistant or intolerant to imatinib.
Sprycel is now approved and marketed worldwide for these
indications in more than 60 countries including the European Union
(EU), Japan and Canada.
Sprycel is also an FDA-approved treatment for adults with newly
diagnosed CP Ph+ CML (since October 2010). Sprycel received
accelerated FDA approval for this indication. The effectiveness of
Sprycel is based on cytogenetic response and major molecular
response rates. The trial is ongoing and further data will be
required to determine long-term outcome. Additional country
approvals for this indication total more than 50.
SPRYCEL® (dasatinib) INDICATIONS &
IMPORTANT SAFETY INFORMATION
INDICATIONS
SPRYCEL® (dasatinib) is indicated for the treatment of adults
with:
- Newly diagnosed Philadelphia
chromosome-positive chronic myeloid leukemia (Ph+ CML) in chronic
phase. The effectiveness of SPRYCEL is based on cytogenetic and
major molecular response rates. The trial is ongoing and further
data will be required to determine long-term outcome
- Chronic, accelerated, or myeloid or
lymphoid blast phase Ph+ CML with resistance or intolerance to
prior therapy including imatinib
IMPORTANT SAFETY INFORMATION
Myelosuppression:
Treatment with SPRYCEL® (dasatinib) can cause severe (NCI CTC
Grade 3/4) thrombocytopenia, neutropenia, and anemia. Their
occurrence is more frequent in patients with advanced phase CML or
Ph+ ALL than in chronic phase CML. Myelosuppression was reported in
patients with normal baseline laboratory values as well as in
patients with pre-existing laboratory abnormalities.
- Perform complete blood counts (CBCs)
weekly for the first 2 months and then monthly thereafter, or as
clinically indicated
- Myelosuppression was generally
reversible and usually managed by dose interruption, dose
reduction, or discontinuation
- Hematopoietic growth factor has been
used in patients with resistant myelosuppression
Bleeding Related Events:
SPRYCEL caused platelet dysfunction in vitro and
thrombocytopenia in humans. In all clinical trials, severe central
nervous system (CNS) hemorrhage, including fatalities, occurred in
1% of patients receiving SPRYCEL. Severe gastrointestinal
hemorrhage, including fatalities, occurred in 4% of patients and
generally required treatment interruptions and transfusions. Other
cases of severe hemorrhage occurred in 2% of patients.
- Most bleeding events were associated
with severe thrombocytopenia. Exercise caution in patients required
to take medications that inhibit platelet function or
anticoagulants
Fluid Retention:
SPRYCEL is associated with fluid retention. In clinical trials,
fluid retention was severe in up to 10% of patients. Severe
ascites, pulmonary edema, and generalized edema were each reported
in ≤1% of patients.
- Patients who develop symptoms
suggestive of pleural effusion, such as dyspnea or dry cough,
should be evaluated by chest X-ray
- Severe pleural effusion may require
thoracentesis and oxygen therapy
- Fluid retention was typically managed
by supportive care measures that included diuretics or short
courses of steroids
QT Prolongation:
In vitro data suggest that SPRYCEL has the potential to prolong
cardiac ventricular repolarization (QT interval).
- In 865 patients with leukemia treated
with SPRYCEL in five phase 2 single-arm studies, the maximum mean
changes in QTcF (90% upper bound CI) from baseline ranged from 7.0
ms to 13.4 ms
- In clinical trials of patients treated
with SPRYCEL (N=2440), 16 patients (1%) had QTc prolongation as an
adverse reaction. Twenty-two patients (1%) experienced a QTcF
>500 ms
- Administer SPRYCEL with caution to
patients who have or may develop prolongation of QTc, including
patients with hypokalemia, hypomagnesemia, or congenital long QT
syndrome and patients taking anti-arrhythmic drugs, other medicinal
products that lead to QT prolongation, and cumulative high-dose
anthracycline therapy
- Correct hypokalemia or hypomagnesemia
prior to SPRYCEL administration
Congestive Heart Failure, Left Ventricular Dysfunction, and
Myocardial Infarction:
Cardiac adverse reactions were reported in 7% of 258 patients
taking SPRYCEL, including 1.6% of patients with cardiomyopathy,
heart failure congestive, diastolic dysfunction, fatal myocardial
infarction, and left ventricular dysfunction.
- Monitor patients for signs or symptoms
consistent with cardiac dysfunction and treat appropriately
Pulmonary Arterial Hypertension (PAH):
SPRYCEL may increase the risk of developing PAH, which may occur
any time after initiation, including after more than one year of
treatment. Manifestations include dyspnea, fatigue, hypoxia, and
fluid retention. PAH may be reversible on discontinuation of
SPRYCEL.
- Evaluate patients for signs and
symptoms of underlying cardiopulmonary disease prior to initiating
SPRYCEL and during treatment. If PAH is confirmed, SPRYCEL should
be permanently discontinued
Embryo-fetal Toxicity:
SPRYCEL can cause fetal harm when administered to a pregnant
woman. Adverse fetal and infant outcomes have been reported from
women who have taken SPRYCEL during pregnancy. Transplacental
transfer of dasatinib has been measured in fetal plasma and
amniotic fluid and has been found to be comparable to those in
maternal plasma.
- If SPRYCEL is used during pregnancy, or
if the patient becomes pregnant while taking SPRYCEL, the patient
should be apprised of the potential hazard to the fetus
- Advise females of reproductive
potential to avoid pregnancy during treatment with SPRYCEL
Nursing Mothers:
It is unknown whether SPRYCEL is present in human milk; however,
dasatinib was present in the milk of lactating rats.
- Because of the potential for serious
adverse reactions in nursing infants, a decision should be made
whether to discontinue nursing or to discontinue SPRYCEL
Drug Interactions:
SPRYCEL is a CYP3A4 substrate and a weak time-dependent
inhibitor of CYP3A4.
- Drugs that may increase SPRYCEL plasma
concentrations are:
- CYP3A4 inhibitors: Concomitant
use of SPRYCEL and drugs that inhibit CYP3A4 should be avoided. If
administration of a potent CYP3A4 inhibitor cannot be avoided,
close monitoring for toxicity and a SPRYCEL dose reduction should
be considered
- Strong CYP3A4 inhibitors (eg,
ketoconazole, itraconazole, clarithromycin, atazanavir, indinavir,
nefazodone, nelfinavir, ritonavir, saquinavir, telithromycin,
voriconazole). If SPRYCEL must be administered with a strong CYP3A4
inhibitor, a dose decrease or temporary discontinuation should be
considered
- Grapefruit juice may also
increase plasma concentrations of SPRYCEL and should be
avoided
- Drugs that may decrease SPRYCEL plasma
concentrations are:
- CYP3A4 inducers: If SPRYCEL must
be administered with a CYP3A4 inducer, a dose increase in SPRYCEL
should be considered
- Strong CYP3A4 inducers (eg,
dexamethasone, phenytoin, carbamazepine, rifampin, rifabutin,
phenobarbital) should be avoided. Alternative agents with less
enzyme induction potential should be considered. If the dose of
SPRYCEL is increased, the patient should be monitored carefully for
toxicity
- St John’s Wort may decrease
SPRYCEL plasma concentrations unpredictably and should be
avoided
- Antacids may decrease SPRYCEL
drug levels. Simultaneous administration of SPRYCEL and antacids
should be avoided. If antacid therapy is needed, the antacid dose
should be administered at least 2 hours prior to or 2 hours after
the dose of SPRYCEL
- H2 antagonists/proton pump
inhibitors (eg, famotidine and omeprazole): Long-term
suppression of gastric acid secretion by use of H2 antagonists or
proton pump inhibitors is likely to reduce SPRYCEL exposure.
Therefore, concomitant use of H2 antagonists or proton pump
inhibitors with SPRYCEL is not recommended
- Drugs that may have their plasma
concentration altered by SPRYCEL are:
- CYP3A4 substrates (eg,
simvastatin) with a narrow therapeutic index should be administered
with caution in patients receiving SPRYCEL
Adverse Reactions:
The safety data reflect exposure to SPRYCEL in 258 patients with
newly diagnosed chronic phase CML in a clinical trial (minimum of
36 months follow up; median duration of therapy was 37 months), and
in 2182 patients with imatinib-resistant or -intolerant CML or Ph+
ALL in clinical trials (1520 patients had a minimum of 2 years
follow up and 662 patients with chronic phase CML had a minimum of
60 months follow up).
The majority of SPRYCEL-treated patients experienced adverse
reactions at some time. Patients aged 65 years and older are more
likely to experience toxicity. In the newly diagnosed chronic phase
CML trial, the cumulative discontinuation rate was 9% with a
minimum of 36 months follow up. In patients resistant or intolerant
to prior imatinib therapy, the discontinuation rate for SPRYCEL at
2 years for adverse reactions was: 15% of patients in chronic phase
CML (all doses), 16% of patients in accelerated phase CML, 15% of
patients in myeloid blast phase CML, 8% in lymphoid blast phase
CML, and 8% in Ph+ ALL. In patients resistant or intolerant to
prior imatinib therapy with chronic phase CML (minimum 60 months
follow up), the rate of discontinuation for adverse reactions was
18% in patients treated with 100 mg once daily.
- In newly diagnosed chronic phase CML
patients:
- The most frequently reported serious
adverse reactions included pleural effusion (4%), hemorrhage (2%),
congestive heart failure (1%), pulmonary hypertension (1%), and
pyrexia (1%)
- The most frequently reported adverse
reactions (reported in ≥10% of patients) included myelosuppression,
fluid retention events (pleural effusion and superficial localized
edema), diarrhea, headache, musculoskeletal pain, rash, and
nausea
- Grade 3/4 laboratory abnormalities
included neutropenia (24%), thrombocytopenia (19%), anemia (12%),
hypophosphatemia (7%), hypocalcemia (3%), elevated bilirubin (1%),
and elevated creatinine (1%)
- In patients resistant or intolerant to
prior imatinib therapy:
- The most frequently reported serious
adverse reactions included pleural effusion (11%), gastrointestinal
bleeding (4%), febrile neutropenia (4%), dyspnea (3%), pneumonia
(3%), pyrexia (3%), diarrhea (3%), infection (2%), congestive heart
failure/cardiac dysfunction (2%), pericardial effusion (1%), and
CNS hemorrhage (1%)
- The most frequently reported adverse
reactions (reported in ≥20% of patients) included myelosuppression,
fluid retention events, diarrhea, headache, dyspnea, skin rash,
fatigue, nausea, and hemorrhage
- Grade 3/4 hematologic laboratory
abnormalities in chronic phase CML patients resistant or intolerant
to prior imatinib therapy who received SPRYCEL 100 mg once daily
with a minimum follow up of 60 months included neutropenia (36%),
thrombocytopenia (24%) and anemia (13%). Other grade 3/4 laboratory
abnormalities included: hypophosphatemia (10%) and hypokalemia (2%)
- Among chronic phase CML patients with
resistance or intolerance to prior imatinib therapy, cumulative
Grade 3 or 4 cytopenias were similar at 2 and 5 years including:
neutropenia (36% vs 36%), thrombocytopenia (23% vs 24%), and anemia
(13% vs 13%)
- Grade 3/4 elevations of transaminase or
bilirubin and Grade 3/4 hypocalcemia, hypokalemia, and
hypophosphatemia were reported in patients with all phases of CML
- Elevations in transaminase or bilirubin
were usually managed with dose reduction or interruption
- Patients developing Grade 3/4
hypocalcemia during the course of SPRYCEL therapy often had
recovery with oral calcium supplementation
Please see the full Prescribing Information at
www.bms.com.
SPRYCEL is a registered trademark of Bristol-Myers Squibb
Company.
Immuno-Oncology at Bristol-Myers
Squibb
Surgery, radiation, cytotoxic or targeted therapies have
represented the mainstay of cancer treatment over the last several
decades, but long-term survival and a positive quality of life have
remained elusive for many patients with advanced disease.
To address this unmet medical need, Bristol-Myers Squibb is
leading advances in the innovative field of immuno-oncology, which
involves agents whose primary mechanism is to work directly with
the body’s immune system to fight cancer. The company is exploring
a variety of compounds and immunotherapeutic approaches for
patients with different types of cancer, including researching the
potential of combining immuno-oncology agents that target different
and complementary pathways in the treatment of cancer.
Bristol-Myers Squibb is committed to advancing the science of
immuno-oncology, with the goal of changing survival expectations
and the way patients live with cancer.
About Bristol-Myers
Squibb
Bristol-Myers Squibb is a global pharmaceutical company whose
mission is to discover, develop and deliver innovative medicines
that help patients prevail over serious diseases. For more
information about Bristol-Myers Squibb, visit www.bms.com, or
follow us on Twitter at http://twitter.com/bmsnews.
Bristol-Myers Squibb Forward-Looking Statement
This press release contains "forward-looking statements" as that
term is defined in the Private Securities Litigation Reform Act of
1995 regarding the research, development and commercialization of
pharmaceutical products. Such forward-looking statements are based
on current expectations and involve inherent risks and
uncertainties, including factors that could delay, divert or change
any of them, and could cause actual outcomes and results to differ
materially from current expectations. No forward-looking statement
can be guaranteed. Among other risks, there can be no guarantee
that Opdivo, or any other compounds mentioned in this release, will
receive regulatory approval in the U.S. or, if approved, that it
will become a commercially successful product. Forward-looking
statements in this press release should be evaluated together with
the many uncertainties that affect Bristol-Myers Squibb's business,
particularly those identified in the cautionary factors discussion
in Bristol-Myers Squibb's Annual Report on Form 10-K for the year
ended December 31, 2013 in our Quarterly Reports on Form 10-Q and
our Current Reports on Form 8-K. Bristol-Myers Squibb undertakes no
obligation to publicly update any forward-looking statement,
whether as a result of new information, future events or
otherwise.
Bristol-Myers Squibb CompanyMedia:Sarah Koenig,
609-252-4145sarah.koenig@bms.comorChrissy Trank,
609-252-3418Christina.trank@bms.comorInvestors:Ranya Dajani,
609-252-5330ranya.dajani@bms.comorRyan Asay,
609-252-5020ryan.asay@bms.com
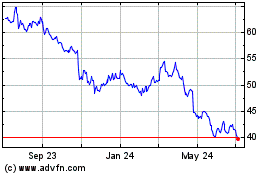
Bristol Myers Squibb (NYSE:BMY)
Historical Stock Chart
From Aug 2024 to Sep 2024
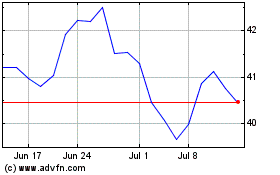
Bristol Myers Squibb (NYSE:BMY)
Historical Stock Chart
From Sep 2023 to Sep 2024