Optum Helping People Stay Connected with Needed Behavioral Health Support During COVID-19
May 11 2020 - 10:00AM
Business Wire
Significant proportions of care shifted to
telehealth by late March
Optum extends telehealth flexibilities through
at least May 31
With a global pandemic continuing to interrupt people’s everyday
lives, access to behavioral health and emotional support has never
been more critical. Optum continues to respond to the need by
significantly expanding the availability of telehealth visits,
including growing the number of providers available to see patients
virtually.
This press release features multimedia. View
the full release here:
https://www.businesswire.com/news/home/20200511005259/en/
(Graphic: Business Wire)
Early data suggests that providers and members are benefiting
from a transition from in-person visits to telehealth sessions
delivered through telephone and video chat platforms, or through
Optum’s proprietary behavioral health virtual visit platform. By
the end of March, 33% of all care was shifted to telehealth with
the following results:
- Behavioral health providers and members have new ways to
deliver or seek care. The more than 200,000 Optum behavioral
health providers are now able to deliver care through alternative
technologies like telephone visits or video chat services. This
policy applies to commercial, Medicare and Medicaid members served
by Optum, and keeps members connected to applied behavior analysis
clinicians, group therapy and intensive outpatient program
sessions. Optum recently extended this flexibility through at least
May 31, 2020.
- Provider participation and member utilization of Optum’s
proprietary behavioral health virtual visit platform are
growing. In March, Optum began to recruit new providers and
accelerate approvals of providers interested in offering virtual
care through its online platform. Since then, the number of
providers participating in this network has increased by more than
45%, bringing the number of certified virtual visit providers to
more than 10,000, and the numbers continue to grow. In addition,
the number of appointments scheduled by members through Optum’s
virtual visit platform is 52% higher than pre-COVID-19
averages.
Early claims data indicates a significant shift in the use of
telehealth for behavioral health care. Normally, about 2% of all
behavioral health claims Optum receives are for a telehealth visit.
By the end of March, approximately 33% of all behavioral health
claims for Optum members were for a telehealth visit. The most
recent claims data indicates that the proportion of telehealth
visits continues to sharply increase.
“We will continue to ensure the people we serve are able to stay
connected with behavioral health care providers during COVID-19,”
said Rebecca Schechter, CEO, Optum Behavioral Health. “We’re also
doing more by proactively reaching out to our most vulnerable
members so they understand how to best continue their treatment,
including prescription refills.”
Additional Optum efforts to serve people needing behavioral and
emotional support include:
- Genoa Healthcare, an Optum business that runs pharmacies
within community behavioral health clinics, has enabled 14
community mental health clinics to use its telepsychiatry platform
to remotely treat their patients. Genoa Pharmacy has shifted to
home and curbside delivery of medications and Genoa's
telepsychiatry is connecting patients with physicians in their
homes to help hundreds access needed psychiatric care. These
efforts are helping ensure Genoa’s 1 million patients, many of whom
are diagnosed with severe mental illness and substance use
disorders, continue to receive treatment.
- Sanvello Health, a UnitedHealth Group company, has made
their premium services free to anyone, and its clinician dashboard
free to professionals during the national crisis. Sanvello is
now ranked the No. 1 app for people looking to manage stress and
anxiety. By the end of March, weekly registrations for Sanvello
were 200% higher than prior averages.
- Optum’s Employee Assistance Program (EAP), serving more than
15 million members globally, is providing members resources they
need online or over the phone. Optum EAP is seeing increased
demand from members seeking emotional, financial and work-life
support, typically four to eight weeks from the peak impact in any
region. The most frequent requests for assistance from members
include addressing opportunities to better manage stress and
anxiety, addressing relationship issues, identifying child or elder
care, and accessing home-schooling resources.
- The free Optum Emotional Support Help Line (866-342-6892)
continues to support people with tips on self-care and connections
to local resources.
Optum behavioral health and EAP members can find more
information by logging on to their Live and Work Well account at
http://www.liveandworkwell.com.
For providers, more information can be found on Provider Express
at www.providerexpress.com.
View source
version on businesswire.com: https://www.businesswire.com/news/home/20200511005259/en/
Aaron Albright 202-383-6403 aaron.albright@optum.com
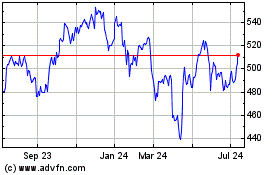
UnitedHealth (NYSE:UNH)
Historical Stock Chart
From Mar 2024 to Apr 2024
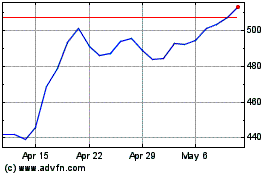
UnitedHealth (NYSE:UNH)
Historical Stock Chart
From Apr 2023 to Apr 2024