- Opdivo is the only PD-1 inhibitor
approved for previously treated metastatic squamous and now
non-squamous NSCLC patients regardless of PD-L1 expression1
- Opdivo represents the only PD-1
inhibitor approved by the FDA to deliver superior overall survival
compared to chemotherapy, docetaxel, in previously treated
metastatic NSCLC1
- Safety profile of Opdivo is consistent
with prior studies1
Bristol-Myers Squibb Company (NYSE:BMY) today announced that the
U.S. Food and Drug Administration (FDA) has approved Opdivo
(nivolumab) injection, for intravenous use, for the treatment of
patients with metastatic non-small cell lung cancer (NSCLC) with
progression on or after platinum-based chemotherapy. Patients with
EGFR mutation or ALK translocation should have disease progression
on appropriate targeted therapy prior to receiving Opdivo. In a
Phase 3 trial, CheckMate -057, Opdivo demonstrated superior overall
survival (OS) in previously treated metastatic non-squamous NSCLC
compared to chemotherapy, with a 27% reduction in the risk of death
(hazard ratio: 0.73 [95% CI: 0.60, 0.89; p=0.0015]), based on a
prespecified interim analysis.1 The median OS was 12.2 months in
the Opdivo arm (95% CI: 9.7, 15.0) and 9.4 months in the docetaxel
arm (95% CI: 8.0, 10.7).1 This approval expands Opdivo’s indication
for previously treated metastatic squamous NSCLC to include the
non-squamous patient population. Squamous and non-squamous NSCLC
together represent approximately 85% to 90% of lung cancer
cases.2
Opdivo is associated with immune-mediated: pneumonitis, colitis,
hepatitis, endocrinopathies, nephritis and renal dysfunction, rash,
encephalitis, other adverse reactions; infusion reactions; and
embryofetal toxicity.1 Please see the Important Safety Information
section below.
“Improving survival for cancer patients represents the ultimate
goal of treatment,” said Murdo Gordon, senior vice president and
head of Worldwide Markets, Bristol-Myers Squibb. “With today’s FDA
approval, it is encouraging to know that Opdivo will be available
to significantly more patients with metastatic NSCLC, helping to
improve treatment outcomes for patients who have been previously
treated. We hope that our efforts to bring innovative
Immuno-Oncology treatments forward for patients will help increase
survivorship and positively impact the lung cancer community.”
This approval is the third for Opdivo in the United States this
year, and is based on the results of the CheckMate -057 trial, a
Phase 3 trial which demonstrated superior OS benefit for Opdivo vs.
docetaxel in previously treated metastatic NSCLC. Opdivo is the
only PD-1 therapy to have been studied in a Phase 3 trial of
patients with previously treated squamous NSCLC and a separate
Phase 3 trial of patients with previously treated non-squamous
NSCLC. Biomarker testing is not required for Opdivo.
“Non-small cell lung cancer is a difficult to treat disease with
high mortality, and patients with squamous and non-squamous NSCLC
often respond differently to treatment,” said Dr. Roy Herbst, Chief
of Medical Oncology, Yale Cancer Center and Smilow Cancer Hospital
at Yale-New Haven. “Opdivo is becoming an important treatment
option for more patients with previously treated metastatic NSCLC,
and is a welcome addition to our therapy of this disease.”
Proven Superior Overall Survival Versus
Docetaxel in Metastatic NSCLC
CheckMate -057 is a landmark, comparative study designed with
the goal of demonstrating survival. Clinical results from CheckMate
-057 were recently presented at the 2015 European Cancer Congress
with simultaneous publication in the New England Journal of
Medicine. CheckMate -057 is a Phase 3, open-label, randomized
clinical trial that evaluated Opdivo (3 mg/kg administered
intravenously every two weeks) (n=292) vs. docetaxel (75 mg/m2
administered intravenously every three weeks) (n=290), in patients
with metastatic non-squamous NSCLC who had experienced disease
progression during or after one prior platinum doublet-based
chemotherapy regimen. Appropriate targeted therapy may have been
given to patients with known EGFR mutation or ALK translocation.1
This study included patients regardless of their PD-L1 (programmed
death ligand-1) expression status. The primary endpoint of this
trial was OS.1
The median OS was 12.2 months in the Opdivo arm (95% CI: 9.7,
15.0) and 9.4 months in the docetaxel arm (95% CI: 8.0, 10.7).1 The
hazard ratio (HR) was 0.73 (95% CI: 0.60, 0.89; p=0.0015), which
translates to a 27% reduction in the risk of death with Opdivo
compared to docetaxel.1 The prespecified interim analysis was
conducted when 413 events were observed (93% of the planned number
of events for final analysis).1 Additional secondary endpoints
include investigator-assessed objective response rate (ORR) and
progression-free survival (PFS). The ORR in the Opdivo arm was 19%
(56/292; 4 complete responses, 52 partial responses) (95% CI: 15,
24) and 12% with docetaxel (36/290; 1 complete response, 35 partial
responses) (95% CI: 9, 17) p=0.02. The median duration of response
was 17 months in the Opdivo arm and 6 months in the docetaxel arm.
Median PFS was 2.3 months in the Opdivo arm vs. 4.2 months with
docetaxel; HR=0.92 (95% CI:0.77, 1.11, p=0.39).
“With today’s announcement, Opdivo represents the only PD-1
inhibitor approved for patients regardless of PD-L1 expression, and
offers significant improvement over the current standard
chemotherapy,” said Michael Giordano, senior vice president, head
of Development, Oncology, Bristol-Myers Squibb. “Through our
leadership in Immuno-Oncology research, we have taken a
comprehensive approach to better understanding and treating
metastatic NSCLC, with a primary focus on patients who are in need
of new options. We are committed to building upon the promise that
Opdivo has demonstrated for patients and providing a potential
survival benefit in devastating diseases, like metastatic
NSCLC.”
The safety profile of Opdivo in CheckMate -057 was consistent
with prior studies. Serious adverse reactions occurred in 47% of
patients receiving Opdivo. The most frequent serious adverse
reactions in at least 2% of patients receiving Opdivo were
pneumonia, pulmonary embolism, dyspnea, pleural effusions and
respiratory failure. Opdivo was discontinued in 13% of patients and
was delayed in 29% of patients for an adverse reaction. The most
common adverse reactions (reported in ≥20% of patients) were
fatigue (49%), musculoskeletal pain (36%), cough (30%), decreased
appetite (29%) and constipation (23%).1
“The approval of Opdivo for patients with previously treated
metastatic NSCLC represents a major advancement in the way we are
able to address the unmet needs of these patients, especially for
those who have progressed on prior treatment and, until now, may
have had limited options,” said Andrea Ferris, president and
chairman of LUNGevity Foundation. “Bristol-Myers Squibb has shown
unwavering commitment to improving survival expectations for
patients with metastatic NSCLC and I applaud their work, along with
the FDA, in making this treatment option available to more
patients.”
Bristol-Myers Squibb has partnered with Dako, an Agilent
Technologies company, to develop PD-L1 IHC 28-8 PharmDx, a test
which was used to assess PD-L1 expression in the CheckMate -057
trial. This test is now approved by the FDA as a complementary
diagnostic, which will provide additional information for
physicians. These tests are distinct from companion diagnostics,
which are essential for safe and effective use of a drug. Biomarker
testing is not required for Opdivo.
About Lung Cancer
Lung cancer is one of the leading causes of cancer deaths in the
United States.2 NSCLC is one of the most common types of the
disease and accounts for approximately 85% to 90% of lung cancer
cases.2 Squamous NSCLC accounts for approximately 25% to 30% of all
lung cancer cases, while non-squamous NSCLC accounts for
approximately 45% to 60% of all lung cancer cases.2 Survival rates
vary depending on the stage and type of the cancer and when it is
diagnosed. For Stage IV NSCLC, the five-year survival rate is one
percent.2
About Bristol-Myers Squibb’s Patient
Support Programs for Opdivo
Bristol-Myers Squibb remains committed to helping patients
through treatment with Opdivo. For support and assistance, patients
and physicians may call 1-855-OPDIVO-1. This number offers one-stop
access to a range of support services for patients and healthcare
professionals alike.
About Bristol-Myers Squibb’s Access
Support
Bristol-Myers Squibb is committed to helping patients access
Opdivo and offers numerous programs to support patients and
providers in gaining access. BMS Access Support®, the Bristol-Myers
Squibb Reimbursement Services program, is designed to support
access to BMS medicines and expedite time to therapy through
reimbursement support including Benefit Investigations, Prior
Authorization Facilitation, Appeals Assistance, and assistance for
patient out-of-pocket costs. BMS Access Support assists patients
and providers throughout the treatment journey – whether it is at
initial diagnosis or in support of transition from a clinical
trial. More information about our reimbursement support services
can be obtained by calling 1-800-861-0048 or by visiting
www.bmsaccesssupport.com. For healthcare providers seeking Opdivo
specific reimbursement information, please visit the BMS Access
Support Product section by visiting
www.bmsaccesssupportopdivo.com.
About the Opdivo Clinical Development
Program
Bristol-Myers Squibb has a broad, global development program to
study Opdivo in multiple tumor types consisting of more than 50
trials – as monotherapy or in combination with other therapies – in
which more than 8,000 patients have been enrolled worldwide.
Indication and Important Safety Information for
OPDIVO® (nivolumab)
INDICATION
OPDIVO® (nivolumab) is indicated for the treatment of patients
with metastatic non-small cell lung cancer (NSCLC) with progression
on or after platinum-based chemotherapy. Patients with EGFR or ALK
genomic tumor aberrations should have disease progression on
FDA-approved therapy for these aberrations prior to receiving
OPDIVO.
IMPORTANT SAFETY INFORMATION
Immune-Mediated Pneumonitis
Immune-mediated pneumonitis or interstitial lung disease,
including fatal cases, occurred with OPDIVO treatment. Across the
clinical trial experience with solid tumors, fatal immune-mediated
pneumonitis occurred in 0.5% (5/978) of patients receiving OPDIVO
as a single agent. In Checkmate 057, immune-mediated pneumonitis,
including interstitial lung disease, occurred in 3.4% (10/287) of
patients receiving OPDIVO including five Grade 3, two Grade 2, and
three Grade 1 cases. Monitor patients for signs with radiographic
imaging and symptoms of pneumonitis. Administer corticosteroids for
Grade 2 or greater pneumonitis. Permanently discontinue OPDIVO for
Grade 3 or 4 and withhold until resolution for Grade 2.
Immune-Mediated Colitis
Immune-mediated colitis can occur with OPDIVO treatment. Monitor
patients for signs and symptoms of colitis. Administer
corticosteroids for Grade 2 (of more than 5 days duration), 3, or 4
colitis. Withhold OPDIVO for Grade 2 or 3 and permanently
discontinue for Grade 4 or recurrent colitis upon restarting
OPDIVO. In Checkmate 057, diarrhea or colitis occurred in 17%
(50/287) of patients receiving OPDIVO. Immune-mediated colitis
occurred in 2.4% (7/287) of patients including three Grade 3, two
Grade 2, and two Grade 1 cases..
Immune-Mediated Hepatitis
Immune-mediated hepatitis can occur with OPDIVO treatment.
Monitor patients for abnormal liver tests prior to and periodically
during treatment. Administer corticosteroids for Grade 2 or greater
transaminase elevations. Withhold OPDIVO for Grade 2 and
permanently discontinue for Grade 3 or 4 immune-mediated hepatitis.
In Checkmate 057, one patient (0.3%) developed immune-mediated
hepatitis.
Immune-Mediated Endocrinopathies
Hypophysitis, adrenal insufficiency, and thyroid disorders can
occur with OPDIVO treatment. Monitor patients for signs and
symptoms of hypophysitis, signs and symptoms of adrenal
insufficiency during and after treatment, and thyroid function
prior to and periodically during treatment. Administer
corticosteroids for Grade 2 or greater hypophysitis. Withhold
OPDIVO for Grade 2 or 3 and permanently discontinue for Grade 4
hypophysitis. Administer corticosteroids for Grade 3 or 4 adrenal
insufficiency. Withhold OPDIVO for Grade 2 and permanently
discontinue for Grade 3 or 4 adrenal insufficiency. Administer
hormone replacement therapy for hypothyroidism. Initiate medical
management for control of hyperthyroidism. Adrenal insufficiency
occurred in 1% (n=555) of patients receiving OPDIVO as a single
agent. In Checkmate 057, Grade 1 or 2 hypothyroidism, including
thyroiditis, occurred in 7% (20/287) and elevated TSH occurred in
17% of patients receiving OPDIVO. Grade 1 or 2 hyperthyroidism
occurred in 1.4% (4/287) of patients.
Immune-Mediated Nephritis and Renal Dysfunction
Immune-mediated nephritis can occur with OPDIVO treatment.
Monitor patients for elevated serum creatinine prior to and
periodically during treatment. For Grade 2 or 3 increased serum
creatinine, withhold OPDIVO and administer corticosteroids; if
worsening or no improvement occurs, permanently discontinue OPDIVO.
Administer corticosteroids for Grade 4 serum creatinine elevation
and permanently discontinue OPDIVO. In Checkmate 057, Grade 2
immune-mediated renal dysfunction occurred in 0.3% (1/287) of
patients.
Immune-Mediated Rash
Immune-mediated rash can occur with OPDIVO treatment. Monitor
patients for rash. Administer corticosteroids for Grade 3 or 4
rash. Withhold OPDIVO for Grade 3 and permanently discontinue for
Grade 4 rash. . In Checkmate 057, immune-mediated rash occurred in
6% (17/287) of patients receiving OPDIVO including 4 Grade 3
cases.
Immune-Mediated Encephalitis
Immune-mediated encephalitis can occur with OPDIVO treatment.
Withhold OPDIVO in patients with new-onset moderate to severe
neurologic signs or symptoms and evaluate to rule out other causes.
If other etiologies are ruled out, administer corticosteroids and
permanently discontinue OPDIVO for immune-mediated encephalitis.
Across clinical trials of 8490 patients receiving OPDIVO as a
single agent or in combination with ipilimumab, <1% of patients
were identified as having encephalitis. In Checkmate 057, fatal
limbic encephalitis occurred in one patient (0.3%) receiving
OPDIVO.
Other Immune-Mediated Adverse Reactions
Based on the severity of adverse reaction, permanently
discontinue or withhold treatment, administer high-dose
corticosteroids, and, if appropriate, initiate hormone- replacement
therapy. The following clinically significant immune-mediated
adverse reactions occurred in <2% (n=555) of single-agent
OPDIVO-treated patients: uveitis, pancreatitis, abducens nerve
paresis, demyelination, polymyalgia rheumatica, and autoimmune
neuropathy,. Across clinical trials of OPDIVO as a single agent
administered at doses 3 mg/kg and 10 mg/kg, additional clinically
significant, immune-mediated adverse reactions were identified:
facial nerve paralysis, motor dysfunction, vasculitis, diabetic
ketoacidosis, and myasthenic syndrome.
Infusion Reactions
Severe infusion reactions have been reported in <1% of
patients in clinical trials of OPDIVO. In Checkmate 057, Grade 2
infusion reactions occurred in 1% (3/287) of patients receiving
OPDIVO. Discontinue OPDIVO in patients with severe or
life-threatening infusion reactions. Interrupt or slow the rate of
infusion in patients with mild or moderate infusion reactions.
Embryofetal Toxicity
Based on its mechanism of action, OPDIVO can cause fetal harm
when administered to a pregnant woman. Advise pregnant women of the
potential risk to a fetus. Advise females of reproductive potential
to use effective contraception during treatment with
OPDIVO-containing regimen and for at least 5 months after the last
dose of OPDIVO.
Lactation
It is not known whether OPDIVO is present in human milk. Because
many drugs, including antibodies, are excreted in human milk and
because of the potential for serious adverse reactions in nursing
infants from OPDIVO-containing regimen, advise women to discontinue
breastfeeding during treatment.
Serious Adverse Reactions
In Checkmate 057, serious adverse reactions occurred in 47% of
patients receiving OPDIVO. The most frequent serious adverse
reactions reported in ≥2% of patients were pneumonia, pulmonary
embolism, dyspnea, pleural effusion, and respiratory failure.
Common Adverse Reactions
In Checkmate 057, the most common adverse reactions (≥20%)
reported with OPDIVO were fatigue (49%), musculoskeletal pain
(36%), cough (30%), decreased appetite (29%), and constipation
(23%).
Please see U.S. Full Prescribing Information for OPDIVO.
About the Bristol-Myers Squibb and Ono
Pharmaceutical Collaboration
In 2011, through a collaboration agreement with Ono
Pharmaceutical Co., Bristol-Myers Squibb expanded its territorial
rights to develop and commercialize Opdivo globally, except in
Japan, South Korea, and Taiwan, where Ono had retained all rights
to the compound at the time. On July 23, 2014, Bristol-Myers Squibb
and Ono further expanded the companies’ strategic collaboration
agreement to jointly develop and commercialize multiple
immunotherapies – as single agents and combination regimens – for
patients with cancer in Japan, South Korea, and Taiwan.
About Bristol-Myers
Squibb
Bristol-Myers Squibb is a global biopharmaceutical company whose
mission is to discover, develop and deliver innovative medicines
that help patients prevail over serious diseases. For more
information about Bristol-Myers Squibb, visit www.bms.com, or
follow us on Twitter at http://twitter.com/bmsnews.
Bristol-Myers Squibb Forward Looking Statement
This press release contains "forward-looking statements" as that
term is defined in the Private Securities Litigation Reform Act of
1995 regarding the research, development and commercialization of
pharmaceutical products. Such forward-looking statements are based
on current expectations and involve inherent risks and
uncertainties, including factors that could delay, divert or change
any of them, and could cause actual outcomes and results to differ
materially from current expectations. No forward-looking statement
can be guaranteed. Forward-looking statements in this press release
should be evaluated together with the many uncertainties that
affect Bristol-Myers Squibb's business, particularly those
identified in the cautionary factors discussion in Bristol-Myers
Squibb's Annual Report on Form 10-K for the year ended December 31,
2014 in our Quarterly Reports on Form 10-Q and our Current Reports
on Form 8-K. Bristol-Myers Squibb undertakes no obligation to
publicly update any forward-looking statement, whether as a result
of new information, future events or otherwise.
References
1. Opdivo Prescribing Information. Opdivo U.S. Product
Information. Last updated: October 9, 2015. Princeton, NJ:
Bristol-Myers Squibb Company.
2. American Cancer Society Web site. “Detailed Guideline: Lung
Cancer (Non-Small Cell).” Available at:
http://www.cancer.org/acs/groups/cid/documents/webcontent/003115-pdf.pdf.
Accessed on September 15, 2015.
View source
version on businesswire.com: http://www.businesswire.com/news/home/20151009005874/en/
Bristol-Myers SquibbMedia:Carrie Fernandez,
609-419-5448carrie.fernandez@bms.comorLaurel Sacks,
609-897-2944laurel.sacks@bms.comorInvestors:Ranya Dajani,
609-252-5330cell: 215-666-1515ranya.dajani@bms.comorBill
Szablewski, 609-252-5864william.szablewski@bms.com
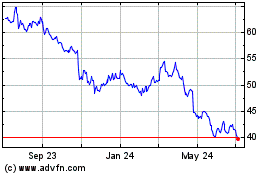
Bristol Myers Squibb (NYSE:BMY)
Historical Stock Chart
From Mar 2024 to Apr 2024
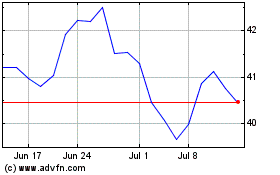
Bristol Myers Squibb (NYSE:BMY)
Historical Stock Chart
From Apr 2023 to Apr 2024